István Roz sos MD, PhD, MBA
sos MD, PhD, MBA
Vascular Surgeon
Specialist of Advanced Chronic Wound Care Techniques
Theta Medical and Aesthetic Centre, Pécs, Hungary
Lecturer at University of Pécs, Hungary
Practical questions, practical answers int the topic of wound treatment - wound healing
........
In the world of guidelines navigation between the various guidelines is slowly becoming the most difficult task for the patient care staff. The reason why the application of the numerous moist wound treatment recommendations poses difficulties is that they convey experience acquired with specific dressing materials and can be converted to our own possibilities only with difficulties. Nonetheless, if we are to embark on this road, comparing our experience leads us to drawing conclusions – hence the existence of practice manuals. During the processing of the numerous important data and significance we can formulate our own practice. Our own theoretical practice! When compiling the present essay I wished to emphasize the importance of practical practice, the practice of „NIL NOCERE” accepted indiscriminately and followed intentionally. Let’s start out with intention. Before embarking on the thematic discussion of wound treatment, let’s stop here for a minute. It cannot be overemphasized that „good intentions” are no substitutes for knowledge, the knowledge of dressing materials, the understanding of the process of wound healing nor can they result in forgiveness for unsuccessful cases either. If there is a lack of the above mentioned things, unfortunately, we have to face not only failure to improve the patient’s condition but the very fact of harming the patient. For this reason I will follow the syllabus of DON’Ts with the presentation of some typical cases.
The disinfection of wounds
The wounds, if of a necrotic nature or if the wound area has a lot of plaque or debris, has to be cleaned physically. This often entails necrectomy, i.e. the surgical removal of the necrotic tissues.
This process cannot be substituted by the recommendation of ’just put it in a solution of sparkling hyperol’ nor with the application of cleansing ointments or gels.
The wound surface and the perilesional area is recommended to be disinfected with efficient but not non-destructive disinfecting solutions. It is important that these solutions should be of standard factory concentration.
Don’t recommend the patient the application of home-made solutions made with neomagnol or hyperol tablets because due to their destructive impact they might have an adverse effect on wound healing and on account of the inaccurate concentration they might even cause serious harm.
The treatment of foot phlegmon of patients with diabetes should be touched upon with a clear emphasis. It may under no circumstances involve the plumbing and irrigation of the area!!! The only chance for healing is the creation of a wide and perspicuous wound surface.
Because of the analgesia the application of irrigation, especially in case of the application of Hyperol, might induce compartment syndrome at the neuropathic, insensitive area and might leave us with no solution other than amputation. In these cases it is not the irreversibility of the inflammation process but the lack of knowledge that results in the amputation of the extremity. Consequently, in the case of the inflamed complication of a diabetic foot plumbing is not an option!
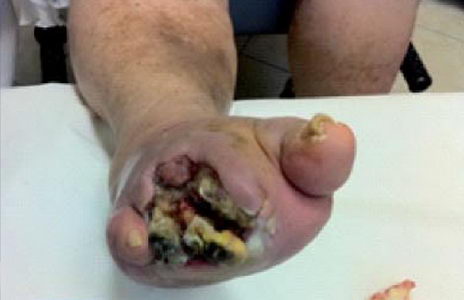
(Figure 1.) Mistreatment of diabetic phlegmon
The foot shown in Figure 1 was saved by necrectomy and the cleansing of the wound with alganates following the quick exploration and the removal of the silicon tubing.
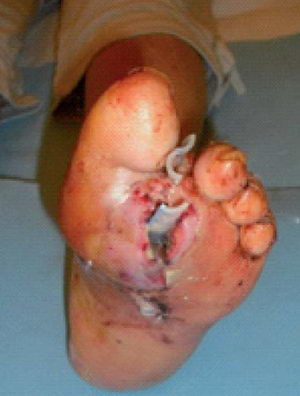
(Figure 2.) Without the removal of the huge amount of necrotic tissues, hyperol rinsing and a little alginate is not enough to keep the process under control
In Figure 2 instead of the surgical removal of the necrotic tissues, rinsing and alginate dressings placed onto the wound surface were supposed to fulfill the requirements of the „moist wound treatment” of healing. Naturally without success. In this case besides the necrotic tissues, the complete removal of the damaged bones was imperatively urgent as well. As expected, the application of suitable alginate dressings on the wound base cleaned in a wide area initiated the healing process properly.
One more thought before changing to the topic of wound covering…
Beside the disinfection of the wounds, the cleanliness of the patient’s environment is to be examined as well. In case we are not convinced that it is intact or if the patient is unable to treat themselves, their temporary accommodation at a family member’s place should also be considered.
Following the creation of the wound base and the disinfection of the wound and the perilesional area, the treatment of the wound with covering materials is carried out.
The healing phases of the wounds and the corresponding development of dressing materials represented a new challenge for healers. While previously the task was the physical protection of the wound surface and the covering of the wound, nowadays wound dressings suited to the pathophysiology of the wound can be applied. Accordingly, it is important even in the case of wound treaters working in groups that only a competent professional should carry out the determination of the type, order and possible combination of dressing materials and the setting of dressing change periods.
Figure 3 and 4 show examples of poor decision-making and implementation, virtually all possible mistakes have been made in one place.
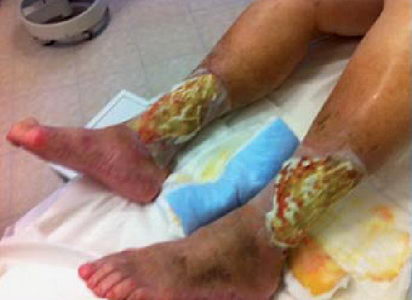
(Figure 3.) Serious mistreatment of a wound with cover dressing still on
In Figure 3 during exposition it can be seen clearly that no compression dressing or stocking has been applied, the dressing fixing, maybe out of economical considerations, fixes the cover dressing only like a sort of patchwork, as a result of which its discharge-absorbing effect cannot be exploited.
Following the removal of this layer – Figure 4 – the alginate layer becomes visible, under which there is an impregnated fabric net on the necrotic wound surface. It is not only a disaster in professional terms but the violation of NHS rules as well.
Never apply epithelization net dressing materials on necrotic wound surfaces.
The dressing fixture should be applied so as to seal the wound properly.
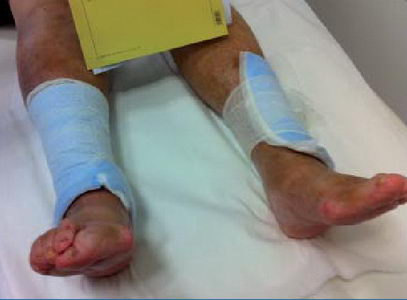
(Figure 4.) Serious mistreatment of a wound following the removal of cover dressing
The terrible pains of the above patient were only conserved by this solution. The huge volume of discharge corroded its environment as well and because of the stagnation improvement of wound status could not be expected.
At this point mistakes the prevention of which is our common goal should be addressed. The application of powders on the wound surface or the covering of the wound surface with ointments or pastes are remnants of the previous mechanic dry wound treatment techniques. Research findings have proved their ineffectiveness and their occasionally damaging effects. It is very important not to apply these so as not to make the further application of moist wound treatment impossible.
The suitable wound dressing
The suitable solution in these cases is the application of foam rubber pads and hydrogels. In addition, a zinc-hyaluronate containing gel (Curiosa®) is recommended in order to improve the efficiency of cover dressings and accelerate epithelization since zinc has superior antibacterial effect to that of silver but has no toxic accumulation, moreover, through its adhesive property hyaluronate facilitates the regeneration process through an arrangement of water structure. No bubbles precipitate from the preparation on the wound surface hindering the healing process as in the cases of ointments and powders. In the course of our previous examinations, the combination of properly chosen dressing materials and Curiosa® gel resulted in the improvement of the healing dynamics of chronic wounds as well as providing the lasting effect of these results.
Due to their special wrapping, following proper training these intelligent wound dressings can be applied in the patient’s home as well. I find it important in my practice that patients with chronic wounds should visit the professional medical treatment facilities with an accompanying person. Being in a stressful situation, the patient cannot memorize every instruction and recommendation and in a lot of cases the anatomy of the wound makes external help necessary as well. In addition to that, if the oedema is treated with a flexible bandage, its proper placement is possible only with assistance.
Figure 5 and 6 illustrate how ostentatious mistakes can be made during wound treatment: the compression bandage or stocking is missing in both cases.
In Figure 5 the necessary dressing change periods were set improperly. The bloody, wet and dirty dressing material poses a great danger for the cleanliness of the wound surface and may result in the corrosion of the perilesional area.
In Figure 6 a scrappy fixing can be observed, it has clearly been veritably patched up. This may fall off even in the course of normal use, and the protection of the wound surface is gone. Let’s not accept solutions like this!
I have referred to the fact several times that in the case of the treatment of a chronic wound situated on the lower extremities the application of compression therapy is inevitable. It can be implemented with the application of a stocking or bandage. In the application of a bandage the rule is as follows: we cannot apply the strip on ourselves properly, therefore only another assisting person can wrap it on properly!
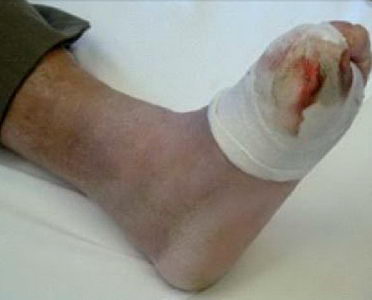
(Figure 5) The result of badly set dressing change period
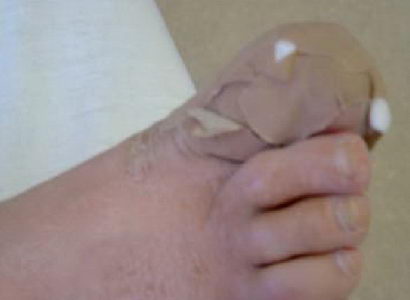
(Figure 6) Sub-standard wound dressing
With the appropriate fixing of the properly chosen cover dressing compression stockings can be applied without any complications. Special multi-layer ulcer stockings are already available.
If the patient uses these tools properly, they retain their proper flexibility and shape for up to a period of half a year. If the patient keeps on insisting that their compression stocking is still good after several terms, be suspicious as they surely do not apply it according to the instructions – and the wound is not healing.
Finally, a closing picture to illustrate what the everyday stocking of a patient may look like, who comes to the doctor for examination with such a ’design’, because they are in the habit of putting on the best-looking one for such occasions (Figure 7).
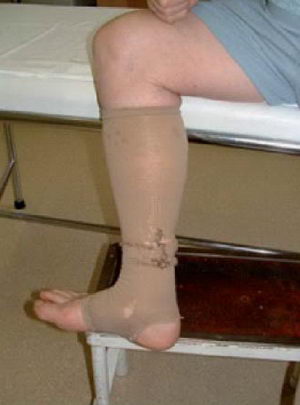
(Figure 7) Compression stocking in a unique condition
Summary
With the discussion of practical questions and the application of the nil nocere principle I wished to hand over Adriane’s string in the labyrinth of wound treatment and wound healing, which is nothing else but an aid helping us to keep on the right track. We have to understand that although higher technology dressings are more efficient, they work only in appropriately competent hands.
Good intentions do not replace knowledge and modern dressing materials can aid us in our healing work only if applied at the appropriate wound stage.
Bibliography
1. Baghel, S. Shukla, R. K. Mathur and R. Randa., A comparative study to evaluate the effects of honey dressing and silver sulfadiazine dressing on wound healing in burn patients, Indian J Plast Surg 42 (2): pp. 176- 181, 2009
2. József Baksa, (2007) Choice of wound dressing, Wound treatment-Wound healing, X, issue 2.. pp. 8-16.
3. Chen Jiong, Han Chun-Mao, Su Guo-Liang, Tang Zhi-Jian, Su Shi-Jie and Lin Xiao-Wei 2007., Randomized controlled trial of the absorbency of four dressings and their effects on the evaporation of burn wounds, Chin Med J 120 (20): pp. 1788- 1791
4. Daróczy J., Rédling M., Telkes M., Ménesi E., Wenzl E., Poroszkai M. (2010) Treatment of non-healing wounds, guiding principles of diagnosis and treatment, Treatment Advice, Academy of Further Education for Physicians Scientific Association, Budapest
5. Dechart A. T. et al: Hyaluronan in human acute and chronic dermal wounds, Wound Rep.REG(2008) 14, pp. 252-258
6. Zsuzsanna Gurzo, Dr. Tibor Rokszin, Curiosin treatment following a minor amputation in diabetes mellitus. Vascular Diseases: 2001/3. pp. 91-95
7. Hollisaz, Mohammad Taghi, Hossein Khedmat and Fatemeh Yari, 2004, A randomized clinical trial comparing hydrocolloid, phenytoin and simple dressings for the treatment of pressure ulcers, BMC Dermatology 4: 18
8. János Hunyadi, (2005) Diagnostics and treatment of diseases causing chronic wounds – A formulation of demand for a several-step treatment model, MOTESZ Magazine, issue 1.pp. 18-24.
9. János Hunyadi, Imre Bihari,Imre Nagy, Zsolt Török, Péter Hamar, (2004)Treatment of chronic wounds in various stages of healing, Vascular Diseases, XI. issue 2.
10. János Hunyadi, Dr.Imre Bihari, Dr.Anna Landi, Dr.László Cervenák, Dr.Szabolcs Rugonfalvi Kiss, Chronic venal insufficiency and ulcus cruris Vascular Diseases: 2004/4. pp. 123-133
11. János Hunyadi, Dr.Imre Bihari, Dr. Imre Nagy, Dr.Zsolt Török, Dr. Péter Hamar- Treatment of chronic wounds in various stages of healing. Vascular diseases: 2004/2. pp. 57-65
12. János Hunyadi, Mária Hok-Salczer,István Sugár (2008) The concept, criteria and principles of treatment of chronic and hard-to-heal wounds as reflected in international and domestic consensus,Wound treatment – Wound healing, XI/ issue 2.
13. István Juhász, Irén Erdei, (2006) Our experience with antimicrobial nanochrystal dressing with silver content in the local treatment of burns and other wounds, Hungarian Traumatology, Orthopedy, Hand Surgery, Plastic Surgery, year 49 issue 4. pp. 369-377
14. Kotz P., Fisher J., Mccluskey P., Hartwell Sd., Dharma H. 2009, Use of a new silver barrier dressing, ALLEVYN Ag in exuding chronic wounds, Int Wound J 6: pp. 186-194
15. Zoltán Kökény,Péter Hanga, Zsuzsanna Karap-Foki, (2008) The role of wound discharge and dressings, Wound Treatment – Wound Healing XI. issue 1. pp. 9-16.
16. László Mecseki, (2009) Common effort to save extremities with diabetes, Medicus Anonymus issues 7-8. pp. 21-23.
17. I. Rozsos, J. Ferenczy, Sz. Szabó et al.: Endovenous Laser Therapy (EVLT)in the treatment of ulcus cruris 2008. Wound Treatment – Wound Healing XI. issue 1. p. 4.
18. I. Rozsos , The possibility of treatment of chronic wounds and perilesional skin area with Curiosa gel Wound Treatment-Wound Healing 2011 XIV issue 2. p. 6.
19. István Sugár (2008) Disputes on dressings, Wound Treatment- Wound Healing, XI. issue 1.
20. Gábor Szabad, (2010) Up-to-date wound treatment, Review for Further Education of General Practitioners, 15: pp. 276-281
21. Veves Aristidis Md, Peter Sheelan Md, Han T. Pham, A randomized, controlled trial of Promogran (a collagen/oxidazed regenerated cellulose dressing) vs. standard treatment in the management of diabetic foot ulcers, Arch Surg 137: pp. 822-827, 2002
22. Wynne, Roshelle, Mari Bott i, Hilary Stradam, Linda Holsworth, Maria Harinos, Olivia Flavell and Christianne Manterfi eld 2004 Effects of three wound dressing on infection, healing comfort and cost in patients with sternotomy wounds: A randomized trial, Chest 125: pp. 43-49